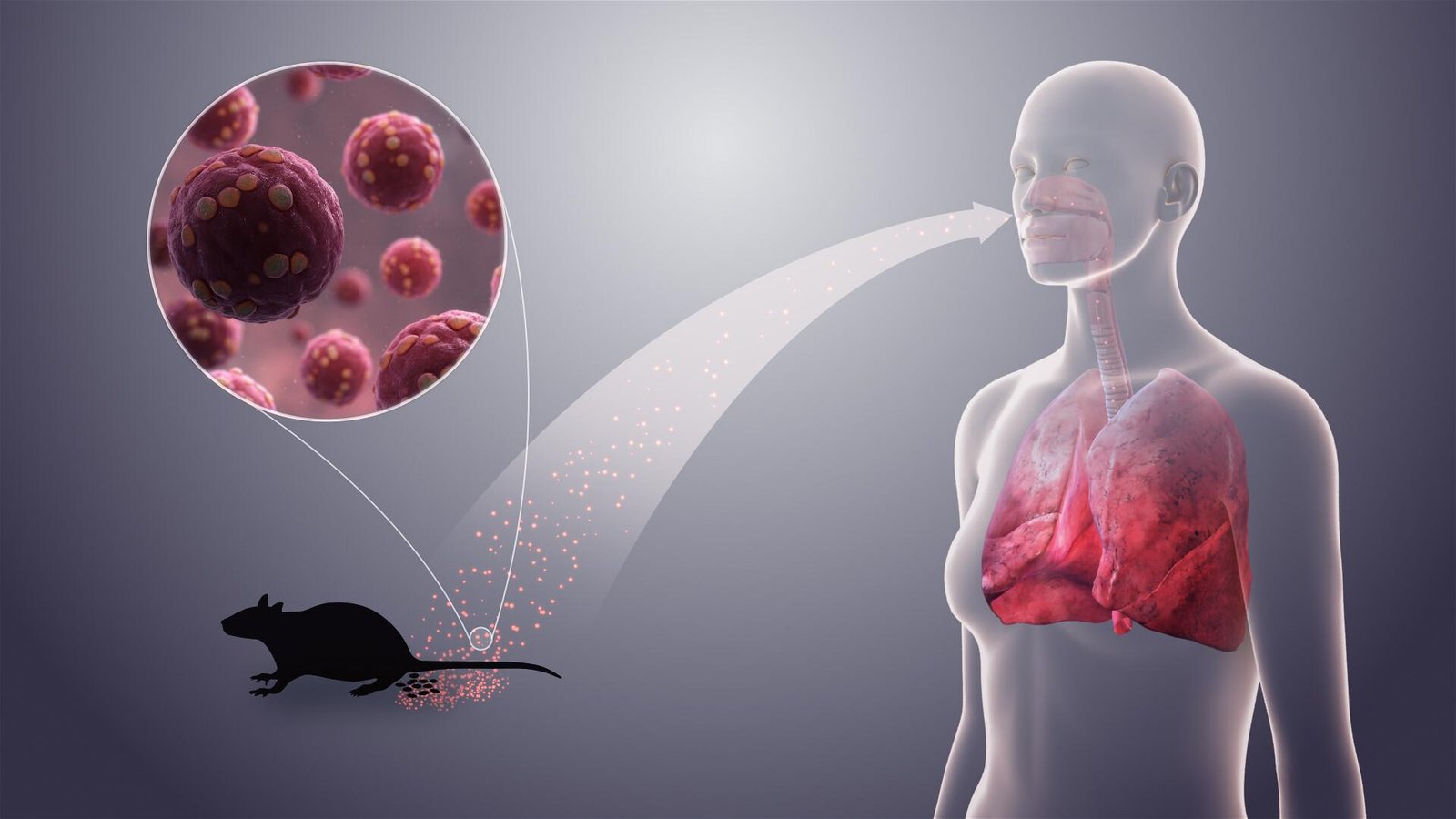
Hantavirus is one of those illnesses people do not think about until they really should. It is not common, but it can be severe, and the early signs often look ordinary enough to fool people. That is part of the danger. The virus is carried mainly by rodents, and infection usually happens when a person breathes in contaminated dust or has contact with rodent urine, droppings, or saliva. In the Americas, some hantaviruses can cause hantavirus cardiopulmonary syndrome, or HCPS, which affects the lungs and heart. In Europe and Asia, hantaviruses can cause hemorrhagic fever with renal syndrome, which mainly affects the kidneys and blood vessels.
The Rodent Link Nobody Loves
The whole story starts with rodents. Not exotic animals. Not a strange mystery source. Ordinary rodents in homes, barns, sheds, cabins, or fields. CDC says hantaviruses are mainly spread from rodents to people, and the virus can get into the air when fresh urine, droppings, or nesting materials are stirred up. WHO says people usually get infected through contact with infected rodents or their urine, droppings, or saliva. That is the core of hantavirus transmission, and it is why dusty cleanups can be risky in a way that is easy to underestimate.
There is one detail worth keeping in mind. Most hantaviruses are not known to spread between people. CDC says the hantaviruses found in the United States are not known to spread person to person, while WHO notes that the Andes virus in South America is the main known exception, with limited human-to-human transmission documented among close contacts. So the situation is serious, but it is not the same as a virus that casually jumps from one person to another in everyday settings.
The First Signs People Miss
The early picture can look bland, almost annoyingly so. Fever. Chills. Headache. Muscle aches. Maybe nausea, vomiting, abdominal pain, or diarrhea. Those are the classic early hantavirus symptoms, and they can show up one to eight weeks after exposure, depending on the virus type. That long gap is one reason people do not connect the dots right away. They remember the dusty garage, the shed, the rodent nest, but they do not think of it until later.
Then things can change quickly. In HPS, cough and shortness of breath may follow, and fluid can build up in the lungs. CDC notes that severe cases can progress to respiratory distress and shock, sometimes very fast. In the United States, the CDC says HPS is fatal in nearly 4 in 10 infected people who develop respiratory symptoms. That number is the reason this disease is taken so seriously, even though it is rare.
How It Spreads In Real Life
The practical version of hantavirus transmission is simple, even if the biology is not. People can get infected by breathing in contaminated air when cleaning areas where rodents have been active. They can also be exposed if saliva, urine, or feces from an infected animal gets into the eyes, nose, mouth, or broken skin. Rodent bites are less common, but they can also spread infection. WHO says activities like cleaning enclosed spaces, farming, forestry work, and sleeping in rodent-infested dwellings increase exposure risk.
That is why the topic is not just about wild animals in remote places. It can be about a cluttered storage room, an old cabin, a garage corner, or a barn where cleaning is rushed, and dry dust goes flying. In a very ordinary-looking room, the danger can be sitting in the wrong place, waiting for movement. That is the real-world shape of hantavirus transmission.
What Doctors Look For
Early diagnosis is tricky because the first illness phase looks like other common infections. WHO says early symptoms can resemble influenza, COVID-19, viral pneumonia, leptospirosis, dengue, or sepsis. That means history matters a lot. Did the person have rodent exposure? Were they cleaning a shed? Did they travel to an area where hantaviruses circulate? Those details help doctors think in the right direction.
Testing usually relies on blood work rather than guesswork. CDC says diagnosis can be made with ELISA tests that detect IgM antibodies, along with rising IgG titers, immunohistochemistry, or PCR, depending on the setting. WHO also notes that laboratory confirmation can use serology or RT-PCR during the acute phase. So the point is not just to recognize the illness clinically. It is to confirm it quickly enough to act.
What Treatment Actually Means
Here is the blunt part. No cure wipes out hantavirus the way people sometimes imagine with viral illnesses. CDC says there is no specific treatment for hantavirus infection, and WHO says there is no licensed specific antiviral treatment or vaccine. Care is supportive. Rest. Hydration. Close monitoring. And when the lungs, heart, or kidneys begin to fail, hospital care becomes urgent. That is the real meaning of hantavirus treatment. It is not a pill that fixes everything. It is rapid supportive medicine that tries to keep the body stable while it fights.
For severe HPS, CDC says treatment may involve oxygen, careful fluid management, intubation, ventilation, and sometimes ECMO in the most serious cases. WHO says early access to intensive care improves outcomes, especially for patients with hantavirus cardiopulmonary syndrome. So timing matters. A lot. The earlier the medical team sees the problem, the better the odds tend to be. That is the hard truth behind hantavirus treatment.
How To Lower The Risk
Prevention is where people have the most control, and honestly, this is where the advice becomes very concrete. CDC says the best prevention is avoiding exposure to rodents and their urine and feces. WHO adds that clean homes and workplaces, sealed entry points, secure food storage, and safe cleanup practices all matter. The goal is simple. Keep rodents out. Do not stir up contaminated dust. Be careful with old nesting material and droppings. That is the heart of hantavirus prevention.
There are a few specific habits that matter more than people realize. CDC and WHO both warn against dry sweeping and vacuuming rodent droppings because this can put contaminated particles into the air. Dampening contaminated areas before cleaning is safer. Hand hygiene matters too. So does careful handling of blood and body fluids in healthcare settings. The virus is not looking for drama. It is looking for a route in. Hantavirus prevention is mostly about closing that route.
Who Faces Higher Risk
Some people simply have more exposure. Pest control workers. Animal caretakers. Farmers. Forestry workers. People who clean barns, sheds, garages, or rodent-infested spaces. CDC says people who handle and clean up after rodents are at higher risk, and WHO notes that certain activities in rodent-heavy environments raise exposure risk as well. This does not mean those jobs are unsafe by default. It means the habits around them matter a lot. Gloves, safe cleaning, and rodent control are not optional extras. They are part of the job.
When To Take It Seriously
A person does not need to panic over every fever. But a fever plus recent rodent exposure is a reason to pay attention. Add muscle aches, stomach symptoms, or sudden breathing trouble, and the picture becomes much more urgent. CDC says patients with suspected HPS need emergency care immediately, preferably in the ICU, even before diagnosis is confirmed. That is because the disease can move faster than people expect.
Frequently Asked Questions
Can hantavirus symptoms start slowly?
Yes. They often begin like the flu, with fever, headache, muscle aches, and stomach symptoms. Then they can worsen quickly, especially if the lungs become involved. The early phase is exactly why the illness is easy to miss.
Can hantavirus transmission happen between people?
Usually no. CDC says the hantaviruses found in the United States are not known to spread person to person. WHO says person-to-person spread has only been documented for the Andes virus, and even then, it is limited and uncommon.
Is there a cure for hantavirus treatment?
No licensed antiviral cure exists. Care is supportive, meaning oxygen, fluids, monitoring, and intensive care when needed. The earlier the treatment starts, the better the chances tend to be.
What matters most in hantavirus prevention?
Rodent control and safe cleanup. Avoid dry sweeping. Do not vacuum droppings casually. Seal openings, store food securely, and keep dusty, contaminated areas damp before cleaning.
When should someone seek help?
Right away, if there is recent rodent exposure and then fever, muscle pain, vomiting, or any breathing difficulty. Hantavirus can turn serious fast, and waiting is the risky choice.
The Quiet Lesson Behind The Virus
Hantavirus is not common, but rarity does not make it harmless. It is a rodent-borne infection that can begin with ordinary-looking hantavirus symptoms, spread through fairly ordinary household or work exposures, and sometimes become severe very quickly. The good news is that hantavirus transmission is well understood, hantavirus treatment is clear about what to do and how fast to do it, and hantavirus prevention is practical enough that many exposures can be avoided with care. That is the part worth holding onto. Not panic. Just attention. And in a disease like this, attention is not a small thing. It may be the difference between a close call and a hospital bed.