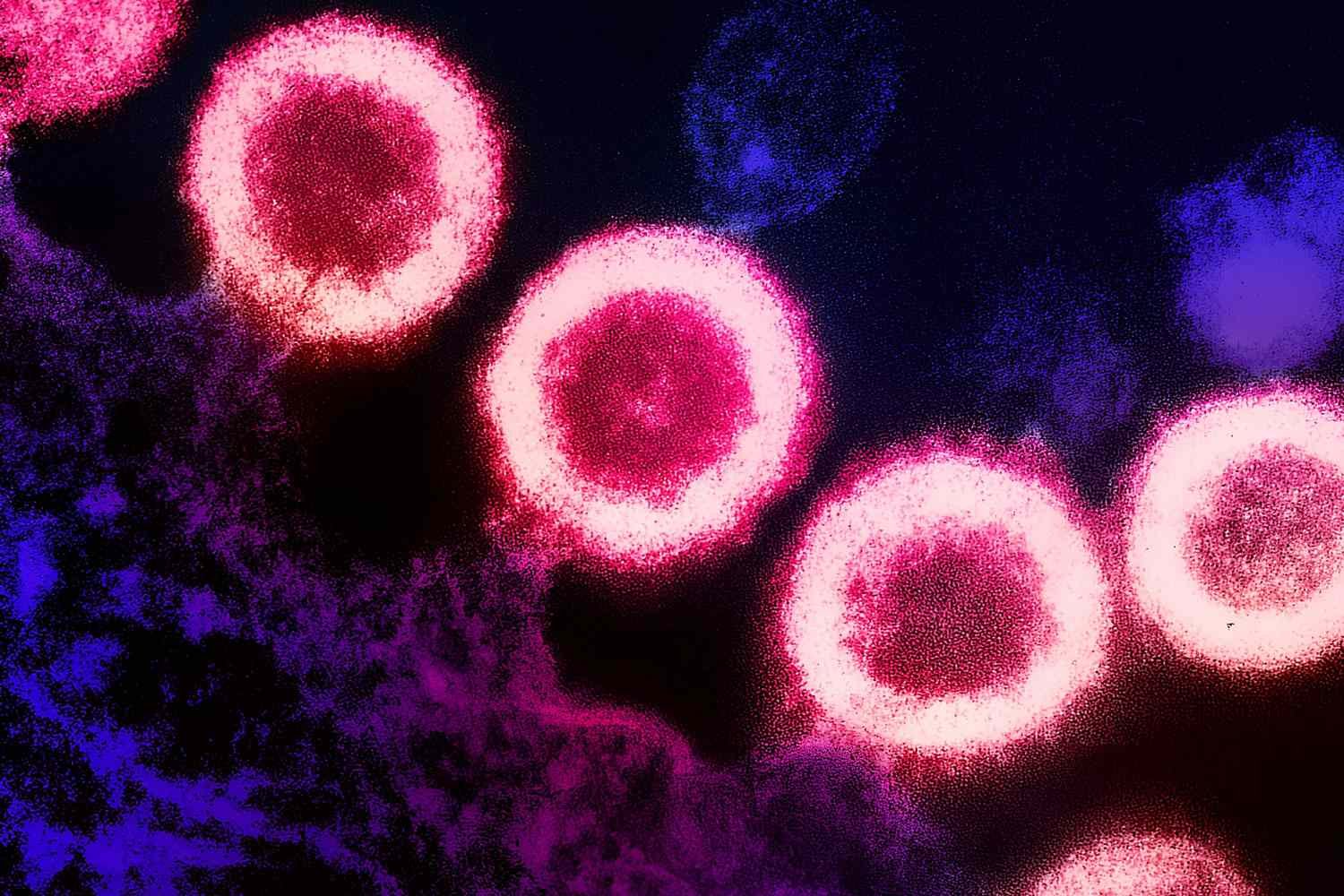
A man from Norway, 63 years old, once treated for blood cancer, has lived without signs of HIV for more than two years post-transplant. His brother gave him stem cells in 2020 – not meant as an HIV cure, but something unusual happened. Those cells held a rare genetic twist, the CCR5Δ32 mutation, unseen at the time of transfer. Gradually, his body rebuilt its defenses using the donated material. Virus levels dropped until tests found nothing. Called the “Oslo patient,” he stands out because most past cases used strangers’ cells from registries. Family donors have never led to this kind of result before. Scientists observe closely, though it remains one of a kind.
Background: HIV and the challenge of a cure
Most people never see it coming – a virus that quietly targets crucial defense cells. This one goes after CD4 helpers, slowly eroding resistance. Left unchecked, protection keeps shrinking. Over time, serious weakness sets in. Eventually, what began subtly may become a full-blown crisis.
These days, medicine lets people with HIV stay well for years. Hidden pockets of the virus survive deep within cells despite treatment. Even though drug control is there, the germs lie quiet, waiting. Full recovery remains out of reach because those hiding spots stick around.
Sticking around so long makes wiping it out a real challenge. Which is exactly what gives someone like the Oslo patient their weight.
Who is the “Oslo patient”?
A man in his sixties from Norway became known as the Oslo patient after doctors found he’d carried HIV since about 2006.
- For years, treatment kept his HIV under control. Still, each day meant sticking to the routine without fail.
- Years after that, his body began struggling to make healthy blood cells because of a rare marrow disorder. This condition, known as myelodysplastic syndrome, slowly took hold where normal cell growth should have been.
- This illness meant swapping out sick bone marrow through a transplant of blood-forming stem cells – a method built for renewal when the body’s factory fails.
Doctors first did the transplant to treat his cancer, not HIV. Yet what happened next surprised everyone.
The key factor: a rare genetic mutation
Why does CCR5Δ32 block HIV entry into cells?
- Most times, HIV sneaks into immune cells once it latches onto something called CCR5 inside the body.
- A few people have a genetic quirk known as CCR5Δ32 – it messes up the CCR5 receptor, leaving it useless. Without a working doorway, most HIV strains find it tough to sneak inside their cells. The door simply does not open the usual way.
In this case:
- From the start, the man’s sibling gave the cells needed. His sister stepped forward when help was required.
- One sibling carried both versions of the CCR5Δ32 change – something that hardly ever happens.
So the body started fresh, its defenses now made of cells that could block HIV.
The transplant process and outcome
Back in November of 2020, the transplant happened.
This is how things unfolded, one piece at a time
1. Replacement of the immune system
After wiping out the faulty bone marrow, doctors put in new stem cells from a donor. Little by little, those fresh cells began their work
- Repopulated his immune system
- Most of the body’s first immune cells got swapped out
Some people call it complete donor chimerism.
2. Removing hidden HIV stores
Researchers tested:
- Blood
- Bone marrow
- Gut tissue
Not a single trace of HIV DNA showed up, not even in spots where the virus tends to linger. Still, deep inside tissues once thought safe, nothing was left behind. Where scientists expected remnants, silence remained. Even hidden corners gave up no clues. What looked like hiding places held space instead.
3. Stopping HIV medication
- Two years post-transplant, treatment ended. Medication ceased then. That pause came well after recovery had settled in. The timeline showed a clear gap between procedure and discontinuation. No doses were taken beyond that point
- He has shown no viral rebound for at least 4–5 years
For now, the virus stays away – that’s what leads researchers to call it a “functional cure.”
What does “likely cured” or “functional cure” mean?
For now, researchers hold back on calling it a cure. They’d rather talk about remission. Progress shows promise – yet conclusions wait. Outcomes improve – but certainty stays distant. Some patients do well – still, doctors keep watch
- Stillness settles where the virus once stirred, now absent without a trace. Treatment stops, yet its silence holds firm. No comeback follows, just a steady absence stretching forward. What was active fades into quiet, unbroken by relapse
- Wipe out every trace of HIV inside a person – total removal, though showing it happened is tough
In the Oslo patient
- No virus has been detected in multiple tissues
- No rebound has occurred after stopping treatment
A clear sign of healing shows up here – yet doctors will watch closely over time. Still, proof points toward recovery even if checks continue.
Just how uncommon could this be?
Most times, you will never see one like it.
- Around the world, just ten people have seen their condition go into remission after a stem cell transplant – one of them lives in Oslo.
Last time, well-known examples were:
- The “Berlin patient” (first cure)
- The “London patient.”
- Several others were treated for blood cancers
What makes this case unique:
- A brother or sister’s match made this treatment possible. The breakthrough came through family tissue alignment.
Why This Isn’t A Cure For All HIV Cases
Even though it works, this method isn’t realistic for many living with HIV.
1. High risk
Stem cell transplants are dangerous:
- Risk of death
- Severe complications like graft-versus-host disease
Complications hit the Oslo patient hard – yet he pulled through. Recovery came slowly, though it did come.
2. When things get really bad, that is when it comes into play
This step usually happens if a person shows these signs:
- Leukemia
- Lymphoma
- Bone marrow disorders
Most won’t use it just for HIV care.
3. Rare donor requirement
Finding a matching donor with:
- Compatible tissue type
- CCR5Δ32 mutation
Why is this case still important?
Still, this example gives useful science lessons despite its limited use. Though narrow in scope, it reveals important details about how things work. A rare situation, yet one that sharpens understanding through careful study.
1. CCR5 involvement confirmed
Blocking CCR5 holds back HIV infection and also stops it from sticking around. Preventing the virus ties closely to cutting off this pathway.
2. Helps understand viral reservoirs
The disappearance of HIV from hidden reservoirs provides clues about:
- How the virus survives
- How it might be eradicated
3. Guides future treatments
Researchers are exploring safer alternatives inspired by these cases:
- Gene editing using CRISPR to copy the CCR5Δ32 mutation
- Therapeutic vaccines
- “Shock and kill” strategies to eliminate the hidden virus
Scientific mechanisms behind the cure
Something probably shifted because of a mix of reasons
1. HIV-resistant immune system
Some fresh immune cells missed a key doorway. That gap shut out the virus, trying again.
2. Conditioning therapy
Chemotherapy before the transplant wiped out diseased cells.
3. Long-term immune reconstitution
Stability arrived slowly, yet the body held its ground against HIV. Resistance settled in without warning. A steady state emerged through quiet persistence.
Broader implications
The biological possibility of curing HIV gains weight because of this instance.
Key takeaways:
- HIV can be eliminated under certain conditions
- The immune system can be engineered to resist infection
- Long-term remission without drugs is achievable
Yet reaching millions still proves tough. Still, getting there involves huge hurdles. Even so, growth at that level brings big problems. Just the same, handling vast numbers feels far off. All the while, expansion on such a scale remains hard. Despite everything, moving into mass use hits roadblocks. In contrast, spreading widely comes with serious limits.
Conclusion
Years now, the man in Oslo lives free of HIV signs – no drugs needed since his transplant. His brother gave bone marrow holding an unusual genetic shift, blocking the virus route. Few others on Earth match this outcome so far. Such heavy medical steps? Too dangerous for most people needing help, though. Still, science gains something solid here – a working example, clear evidence that healing might happen after all. That kind of hope pushes labs toward gentler methods down the road.
FAQs
1. What does it mean that the Norwegian man is “likely cured” of HIV?
A: Years passed without any sign of the virus, even after he stopped taking medicine for HIV. Not seen, not heard – doctors say it’s what happens when the infection goes quiet, a situation they label a “functional cure.” Still, checks go on, just in case something shows up again.
2. What was the reason behind his stem cell transplant to begin with?
A: Doctors performed the transplant mainly because of a severe blood condition known as myelodysplastic syndrome – HIV wasn’t the target. Still, after the procedure, something surprising occurred: the person’s HIV went into remission.
3. For how long has the person stayed clear of HIV while taking no drugs?
A: Years now without medication – about four or five – and still no sign of the virus hiding in his body. That silence inside him makes researchers think he might be one of the few truly free of it.
4. Is it possible for everyone living with HIV to get better using this approach?
A: Most folks with HIV won’t find help here – stem cell transplants come with serious dangers. These procedures show up only when facing deadly illnesses such as cancer. Safety concerns rule them out for everyday use in treating HIV.
5. Why is this case important for future HIV research?
A: One case shows HIV might vanish entirely given the right setup. From moments like these, researchers pull clues – tweaking genes, testing fresh methods – with hope of reaching a fix many could access someday.